How to improve primary healthcare to prepare for future pandemics
These are some of the pivotal areas we need to invest in to build better health systems.
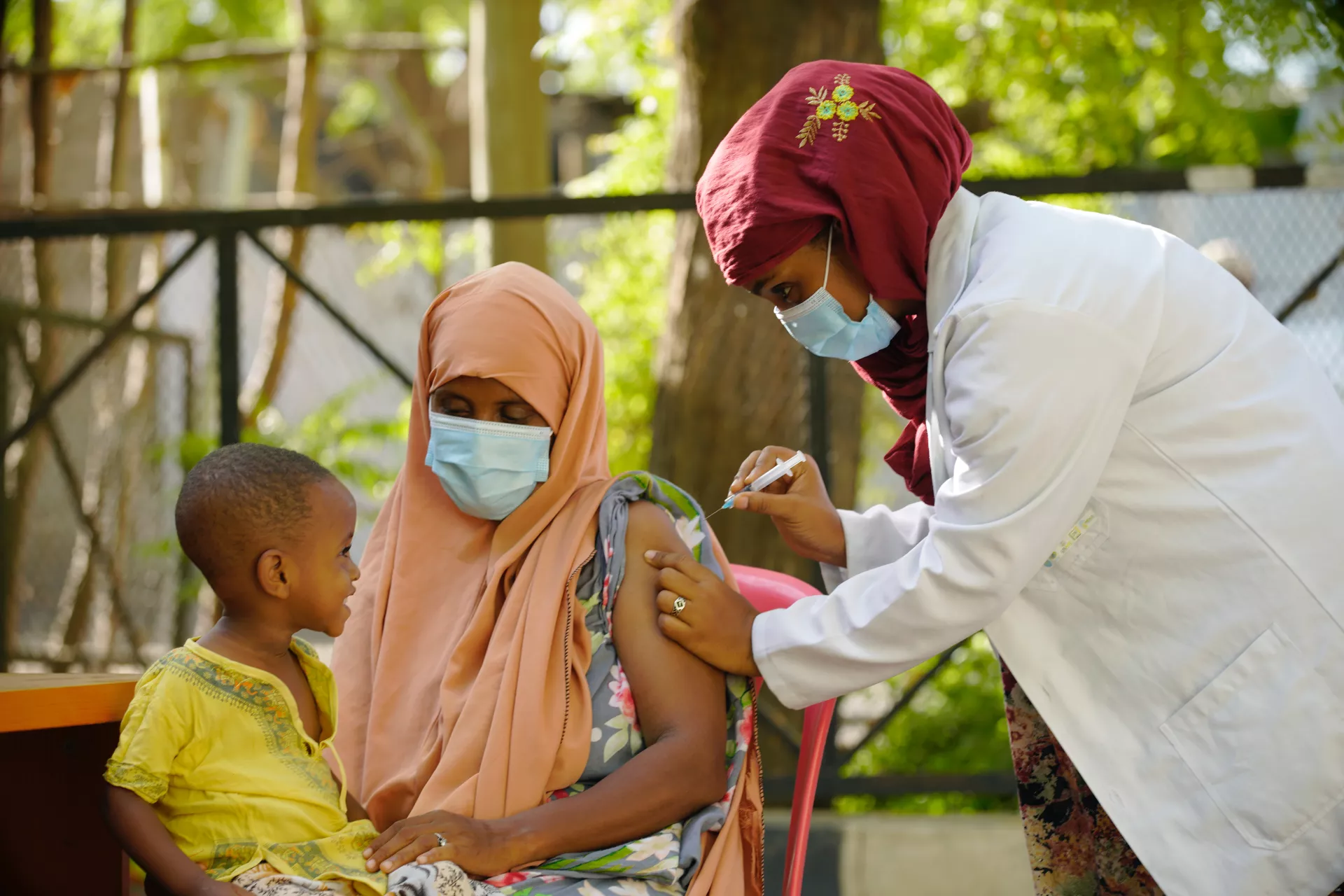
This is the moment to strengthen primary healthcare globally. The COVID-19 pandemic has shown what’s at stake, upending the lives of families around the world. Millions of lives have been lost, while a generation of students faced a learning crisis. It’s been a stark reminder of the need to build resilient health systems globally. Better primary healthcare will help us protect against future pandemics. These are some of the areas to focus on.
1. Recruit, train and prioritize healthcare workers
It goes without saying, healthcare workers are at the heart of any strong healthcare system. Throughout the COVID-19 pandemic, frontline workers, which includes community health workers, have selflessly risen to the challenge. Whether it’s been caring for the sick, making sure that vaccines reach the most vulnerable, testing and reporting cases or keeping routine healthcare services going, their efforts have been immense.
Jennifer Boateng, a pharmacist who works at the Greater Accra Regional Hospital in Ghana, epitomizes the efforts of so many other healthcare workers. “I live with my husband, three children and my mother, who is 80 years old. I was still breastfeeding when I started work at the COVID-19 intensive care unit,” she remembers. “I was truly terrified of contracting the virus and putting my family at risk. Painfully, I had to stop my children from hugging me.”

During the pandemic, Jennifer has been working to make sure that COVID-19 patients get the medication they need. The experience working in the intensive care unit has had a profound impact on her.
“Working here has exposed me to the most deaths I have ever witnessed in my career, a haunting journey that is. Gathering the courage to come to work each morning takes great effort and mental preparation.”
The physical and emotional strain of the pandemic on healthcare workers like Jennifer has been incalculable. To try and protect against future pandemics, healthcare workers must be prioritized more than ever. That means providing them with the necessary training, making sure they’re first in line for vaccines so they’re protected, and financially and emotionally supporting them. That includes building the confidence of healthcare workers, ensuring their thoughts and concerns are understood and working with them to address those issues. This support is needed, not just so that healthcare workers are equipped to do their job properly, but to ensure the profession is an appealing one that can attract and retain talented and dedicated people.
2. Establish effective surveillance and response systems
During the COVID-19 pandemic, clusters of cases have emerged in different parts of the world at different times. New and sometimes more transmissible variants have regularly circulated, and they’ve often spread quickly. With any virus that’s constantly moving and changing, it’s important to have effective testing and reporting mechanisms in place to monitor them. That means that if an outbreak occurs or a new variant emerges, it can be flagged quickly to a central health authority. By raising the alarm quickly, effective measures can be quickly put in place to help limit virus transmission. This kind of surveillance is best when it's done at a community level.

Moving forward, larger investments are needed to improve testing, particularly at the community level, as many low- and middle-income countries still have limited access to and capacity for testing. Until that is in place, our ability to detect and contain future outbreaks will be limited. That means the possibility of more lockdowns with schools and businesses closed. As we know, the social and economic effects of those closures are enormous.
3. Build confidence in health services through community health
When it comes to giving people the vaccines they need to stay healthy and thrive, trust is crucial. Building confidence in healthcare workers, health institutions and national health agencies is therefore key, as that’s where the critical information comes from. By building trust and making sure the guidance from these sources is evidence-based and respected, we can help prevent future pandemics.
On top of trust, it's important to communicate effectively with the public about the healthcare services that are available to them. People need to know that vaccines are available, as well as information like where to go to get the doses and when vaccination workers will be administering them. That’s particularly crucial in rural communities where temporary clinics often provide these services.
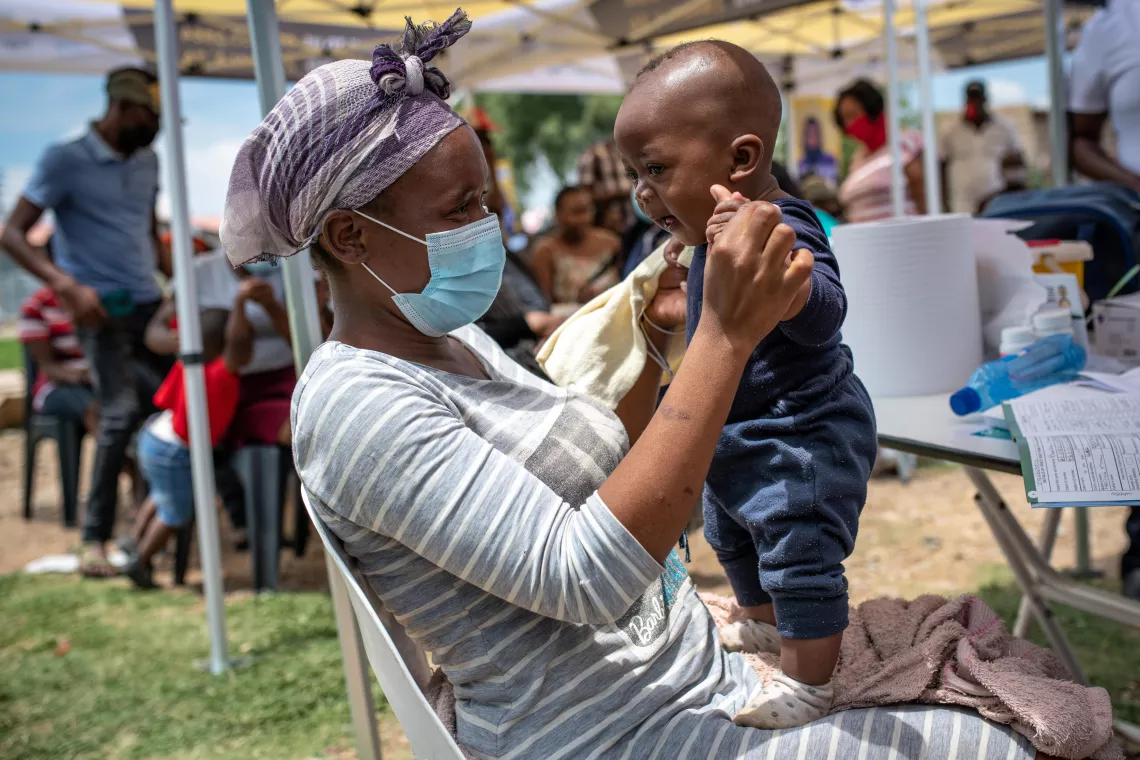
The “Zwakala” vaccine campaign in South Africa is an example of what can happen when trust is combined with effective messaging. The phrase “Zwakala” in Zulu means “come on over,” and it’s often used by friends as an invitation. Through this initiative, community healthcare workers have been mobilizing in parts of the country that had a slow initial COVID-19 vaccination rate. They’ve been communicating through various mediums, whether it’s on local radio, handing out leaflets or speaking face-to-face with members of their community. You can learn more about that campaign and how it’s an example of the need to build trust.
4. Include COVID-19 vaccines in routine immunization packages
To protect communities from COVID-19, vaccines need to be easily accessible at a community level. To achieve that, COVID-19 vaccines will need to be readily available as part of routine immunization packages. That means they’re offered to people as part of a regimen of vaccines throughout their lifetime. This requires expanding and strengthening routine immunization and primary healthcare services to be able to serve adults, while protecting childhood immunization.

5. Strengthen logistics and supply
Developing, delivering and administering COVID-19 vaccines has been a tremendous logistical and supply challenge during the pandemic. But vaccinations require much more than just vaccine doses. Think about the other supplies that have been needed. There’s protective gear, including gloves and masks, that have been essential to keep healthcare workers safe. There’s also the supply of syringes and the cold chain storage that’s been necessary to make sure that the vaccines are stored at the proper temperature and don’t go to waste.
The Philippines is one example of just how important the cold chain storage is when it comes to reaching remote communities with vaccines. The country consists of hundreds of hard-to-reach islands and disaster-prone regions. That includes the municipality of Kabugao, nestled in the mountains, north of the capital, Manila. Extreme flooding is common and the power often goes out. That’s created a particular challenge: making sure the vaccines aren’t wasted when electricity is lost. Thanks to a partnership between UNICEF and the Japanese government, dozens of solar powered refrigerators have been supplied to communities like Kabugao, to make sure that doses last even when the electricity is lost.
Moving forward, increased investments in this kind of infrastructure will help to ensure communities receive the vaccines they need and protect them from future outbreaks.
This is a unique moment where we have an opportunity to not just end this pandemic, but also prevent ones in the future. It’s important that the legacy of COVID-19 is not one of disruption and disparity, but instead a moment of monumental change. That change requires a relentless commitment to strengthening primary healthcare.
Through that commitment to better primary healthcare at both a national and community level, we can build stronger health systems that are equipped for any epidemic or pandemic.

