Cholera is endangering children globally
Learn why outbreaks are occurring and how UNICEF is responding.

Cholera doesn't know borders. Despite being preventable and easily treatable, children continue to suffer from the potentially fatal disease. After years of steady decline, cholera has made a devastating comeback.
Over the past two years, cholera cases have more than doubled. More than 1.1 billion people are at risk, with children under 5 especially vulnerable.
Intestinal infection often spreads because of a lack of clean water and sanitation facilities. Children living in volatile and unstable communities are particularly at risk. Thankfully, vaccines and treatments are available. UNICEF is working to make sure that these provisions reach the children that need them the most. The goal is to make sure that by 2030 cholera is no longer a threat to public health.
Here's what you need to know about cholera and the efforts to eliminate the disease.
What is cholera?
Cholera is an intestinal infection. It’s caused by ingestion of food or water that’s contaminated with the bacterium Vibrio cholerae. Researchers conservatively estimate that every year, there are as many as 4 million cholera cases globally and as many as 143,000 deaths. Young children, especially those under the age of 5, bear the brunt of the disease. Furthermore, malnourished children are more vulnerable to experiencing severe symptoms. Cholera is a preventable and easily treatable disease.
What makes a country cholera-endemic?
A cholera-endemic area is where cases have been detected during the past 3 years, and there’s evidence that it was caused by local transmission, rather than being imported from elsewhere. Meanwhile, a cholera outbreak (epidemic) can occur in countries where cholera does not regularly occur or in endemic countries.

How does cholera spread?
Cholera disproportionately affects the world’s poorest and most vulnerable communities. A lack of access to clean water and sanitation facilities is closely linked to an increased likelihood of cholera transmission. That means that children who are living in urban slums and camps for internally displaced people or refugees are particularly vulnerable. That’s because the minimum requirements of clean water and sanitation are sometimes not met. Poor water management, increased poverty and conflicts make safe water more and more scarce. Between 2010 and 2021, almost all cholera cases – 97 per cent – were seen in countries with the lowest levels of water and sanitation services.
Climate change also contributes to the spread of cholera. Significant rainfall and flooding, which is becoming more frequent, results in an intensified water cycle. That in turn affects access to clean water in communities already vulnerable to these events. Consequently, families and their children often rely on unsafe water, which exposes them to greater risk of contracting the water-borne disease.
If a child is infected with cholera, what are the symptoms?
Most children infected with cholera will have no or mild symptoms, and through the use of oral rehydration solution, they can be successfully treated. But if left untreated, the disease can kill within hours. Severe cases of cholera require rapid treatment with intravenous fluids and antibiotics.
After ingesting contaminated food or water, it can take between 12 hours to 5 days before a child begins to show symptoms. The bacteria remain in the faeces for up to 10 days after infection and is shared back into the ecosystem, which could lead to other people potentially being infected. Cholera can cause acute watery diarrhoea with severe dehydration, which can prove to be fatal. When experiencing diarrhoea, infants and children are at greater risk of dehydration compared to adults, and more so if they are malnourished.
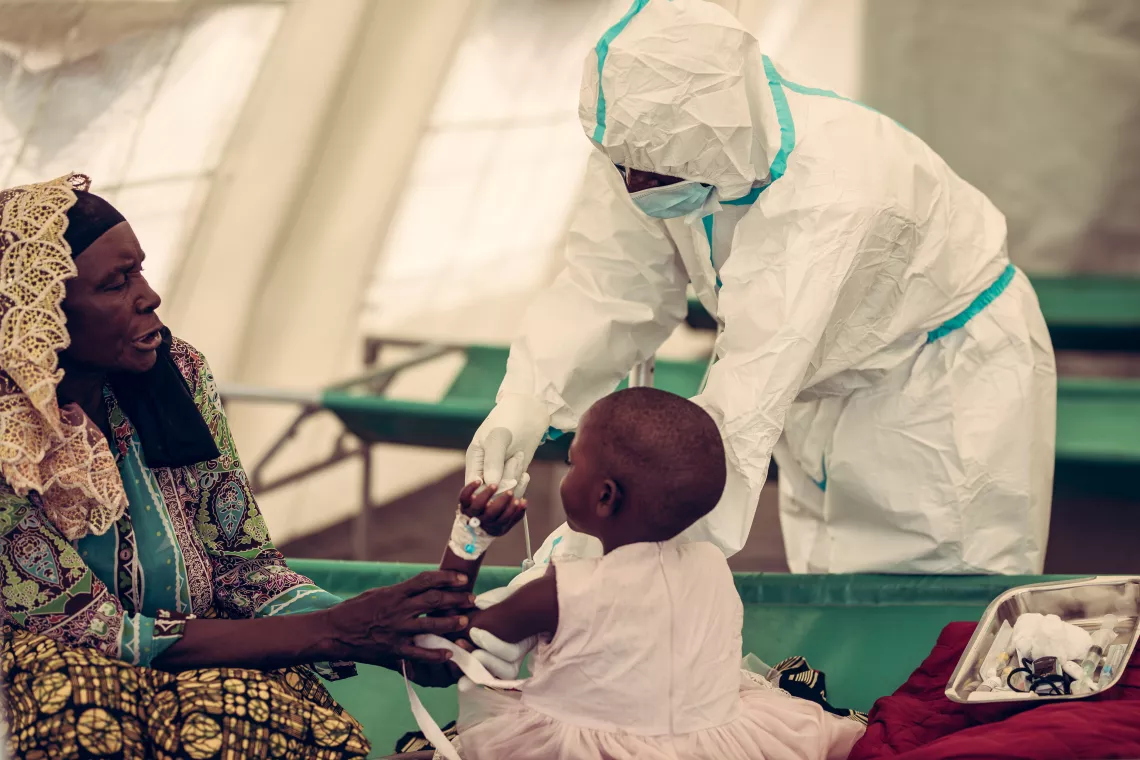
How is cholera treated?
If infected with cholera, most children can be treated successfully through the quick administration of oral rehydration solution (ORS), which is a mixture of salt and sugar. UNICEF and the World Health Organization distribute sachets of this solution that need to be dissolved in clean water.
From 2000 to 2021, the total annual number of deaths from diarrhoea among children under 5 decreased by 64 per cent.
This decline can be linked to the expanded use of ORS for diarrhoea treatment.
If a child is severely dehydrated, treatment beyond oral rehydration solution is necessary. In this instance, intravenous fluids should be rapidly administered, and the child may also require antibiotics to reduce the duration of diarrhoea.
During a cholera outbreak, it is crucial that these treatments are readily accessible. That requires distributing oral rehydration solution to treatment clinics in communities that are significantly impacted. If treated early and properly, the fatality rate can be reduced dramatically.
For children under the age of 5, zinc is an important adjunctive therapy. Zinc is a vital micronutrient that becomes drained during diarrhoea. When given as a supplement, it reduces the duration and severity of the illness, and can also reduce the risk of recurrences in the short term.
What can be done to prevent the spread of cholera?
A multifaceted approach is key to controlling cholera and reducing deaths. First and foremost, ensuring that every child has access to safe drinking water and adequate sanitation is essential. It’s also important that children in communities at risk have access to the WHO pre-qualified oral cholera vaccines.
Furthermore, community engagement plays an important role. Effective and engaging programmes can help to promote protective hygiene measures such as handwashing with soap and the safe disposal of faeces.
Additionally, given that cholera is an easily treatable disease, quick access to treatments during an outbreak, including oral rehydration solution, zinc and antibiotics is crucial. With early and proper treatment, the fatality rate should remain below one per cent.
Effective surveillance systems are also necessary to monitor and control the spread of cholera. The surveillance data gathered should be translated into accessible information that can be used effectively at a local, national and global level.
Are there vaccines available to prevent cholera?
There are currently five World Health Organization pre-qualified oral cholera vaccines: Dukoral, Shanchol, Euvichol, Euvichol-P, and Euvichol-S. In order to be fully protected, all of these vaccines require two doses. The International Coordinating Group (ICG), which UNICEF is a member of, manages the global stockpile of oral cholera vaccines. The group has conducted mass vaccination campaigns resulting in more than 100 million doses of oral cholera vaccines being administered. These campaigns have focused on areas experiencing an outbreak, particularly in highly endemic areas known as “hotspots” and in areas at increased vulnerability during humanitarian crises.
Where is cholera most commonly found?
Over the past two years, cholera cases have more than doubled globally, from 223,370 cases reported in 2021 to 535,321 cases in 2023, and the trend is not slowing down. In 2024, large outbreaks of suspected and confirmed cases of cholera have been reported by several countries, including Democratic Republic of the Congo, Ethiopia, Somalia, Yemen, Afghanistan, Comoros, Pakistan, Syria, Zimbabwe, Zambia and Sudan.
In 2023, Democratic Republic of the Congo experienced the worst cholera outbreak in more than half a decade, with over 8,000 children under five infected in North Kivu during first seven months of the year. This dramatic figure represents more than six times the number of cases reported in all of 2022.
UNICEF is working tirelessly to respond to outbreaks across impacted countries and regions.

How is UNICEF responding to the outbreak of cholera?
UNICEF has stepped up efforts to respond to cholera outbreaks in coordination with national authorities and partners. This includes widely distributing millions of water treatment tablets to ensure families in impacted communities have access to safe water.
We also supply local health departments with oral rehydration salt sachets and zinc, in addition to providing acute watery diarrhoea kits to treat moderate and severe cases. Additionally, UNICEF is increasing access to ready-to-use therapeutic food, as malnutrition is a leading cause of death from cholera.
We’re also helping frontline workers in communities experiencing outbreaks. UNICEF trains these workers in cholera awareness, including transmission, symptoms, treatment and prevention mechanisms. Furthermore, we’re airing prevention information on local radio and TV stations to raise awareness about the situation.
UNICEF uses its deep-root presence in local communities to raise awareness on cholera, engage discussions with leaders and their communities on cholera prevention, and treatment, setting up oral rehydration points (ORPs) and promoting healthier routines.
Furthermore, UNICEF is working to pilot and identify climate-informed and environment-informed approaches that can support in mitigating outbreaks and minimizing their spread when they occur.
These are just a few of the extensive steps and provisions UNICEF adopts to respond to the threat of cholera.
Are we close to eliminating cholera?
Through the successful adoption of prevention measures and increased access to cholera treatment methods, including oral rehydration salt and zinc, we’re closer than ever to ensuring that no child dies from this preventable disease.
In 2023, UNICEF distributed over 1.1 billion water purification tablets, more than 41 million oral rehydration salt sachets and nearly 30,000 cholera kits worldwide.
But these outbreaks that we continue to witness prove that cholera still presents an immediate and potentially grave danger to families, particularly in unstable and volatile communities worldwide.
Worryingly, as outbreaks become more regular and demand for supplies increases, we’re seeing a shortage in essential cholera commodities, including oral rehydration salts and rapid diagnostic kits. At the same time, the global stockpile of oral cholera vaccines is significantly depleted.
To overcome this global emergency, in the immediate term we must reach affected populations to prevent and control cholera through humanitarian action. In the longer term, we need to invest in strengthening water and sanitation systems to prevent future outbreaks.
Despite the challenges that exist, in coordination with our partners, UNICEF has a global strategy that provides a concrete path toward a world in which cholera is no longer a threat to public health. As the recent cholera outbreaks demonstrate, a recommitment to realize this goal is more urgent than ever.




