Child Survival and Development
Giving children a chance to survive and thrive
- English
- Portuguese
Situation and Challenges
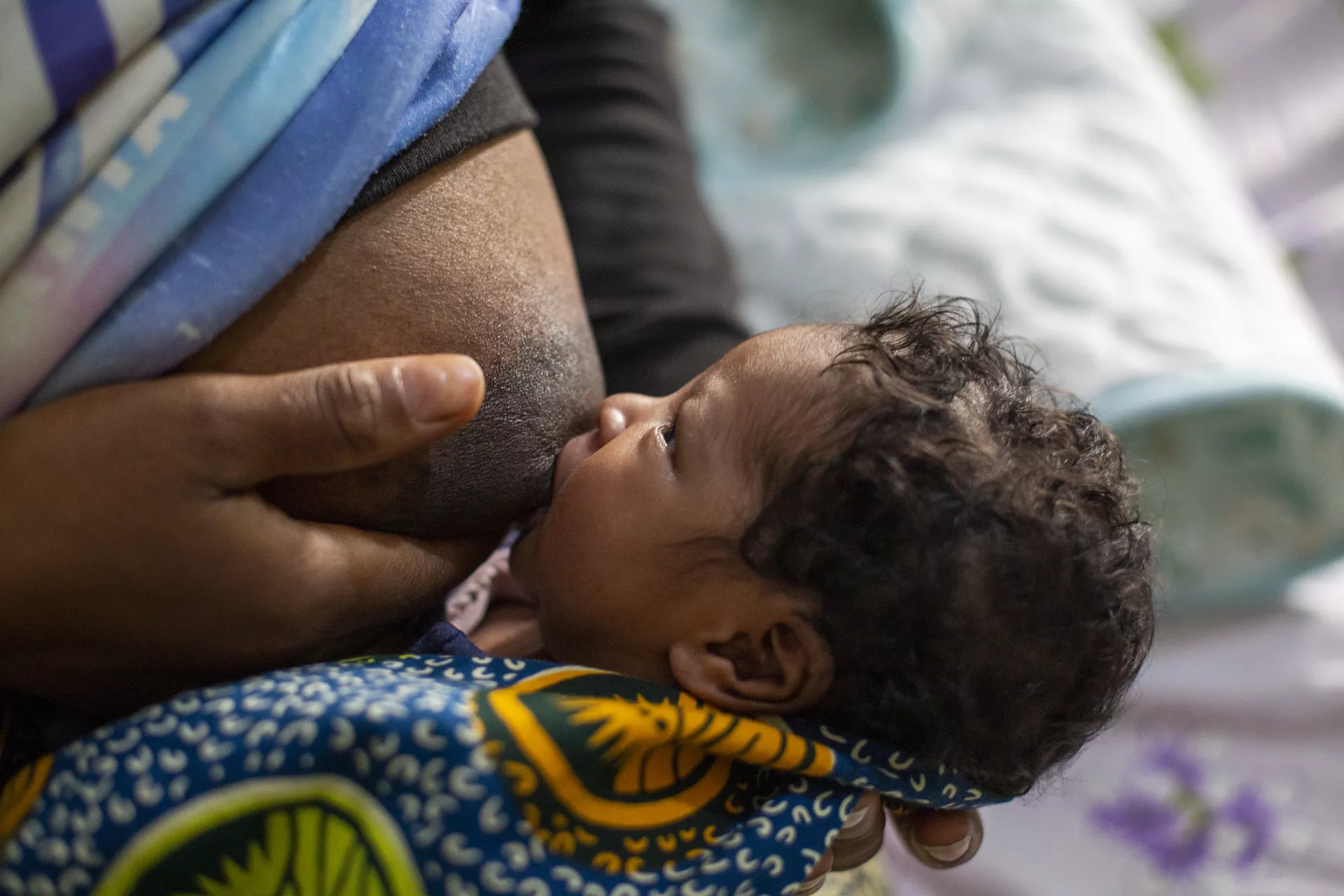
Although child mortality reduced from 89 deaths per 1,000 live births in 2014 to 51 per 1,000 live births in 2019, this decline may have been reversed in 2022. The focus on the COVID-19 response, health worker strikes, frequent stock-outs of vaccines and essential medicines, governance limitations, and inadequate investments, particularly at community level, meant that many pregnant women, new mothers, infants and young children have had restricted access to essential maternal and child health services in the most recent years.
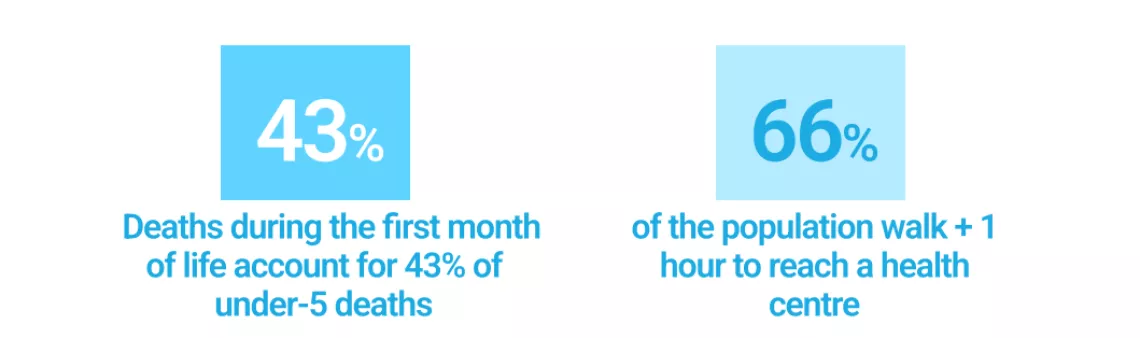
The most recent data shows that deaths during the first month of life account for 43 per cent of under-five deaths, significantly higher than the average for West Africa and sub-Saharan Africa.1 Moreover, Guinea-Bissau has one of the world’s highest maternal mortality ratios (MMR) estimated at 667 per 100,000 live births.2 Over a third (36 per cent) of births are to mothers under 20 and three-quarters of births are to mothers who have previously given birth less than two years earlier.3
Many women and children lack access to health services, and when they do manage to reach a health service, the quality of care is often lacking.
About 66 per cent of the population has to walk more than one hour to reach the nearest health centre, particularly in sparsely populated regions such as Bafatá and Gabú,4 and in 2022, only 61 per cent of births were assisted by skilled health personnel though increasing from 42 per cent in 2021. Road conditions, which are generally poor, were further degraded by intense rains in 2022, hindering access to remote villages for about four months of the year.
Preventable diseases such as malaria, diarrhoea and pneumonia remain major child killers, accounting for 27 per cent of deaths of children under the age of 5. Children are particularly at risk in urban areas, where 65 per cent of unvaccinated children live. The low immunization level is mainly due to inadequate planning and financing of the outreach services for the Expanded Programme on Immunization (EPI), health worker strikes and vaccine stock-outs.
In 2022, a measles outbreak with 214 confirmed cases and 12 fatalities compounded a polio outbreak which had previously occurred in October 2021 with four cases confirmed in the capital, Bissau, and the Biombo region. Encouragingly, a decline in diphtheria, tetanus and pertussis/whooping cough (DPT3) coverage was reversed; coverage had fallen from 74 per cent to 71 per cent between 2020 to 2021 but in 2022 it rose to 78 per cent.

Tamara works in one of the most challenging areas, in the Bijagós archipelago, a group of islands and islets spread across 2,500 square kilometres of the Atlantic off the coast of Guinea-Bissau. She was in one of the 26 vaccination teams walking long distances to ensure that all children were vaccinated. There were reports of vaccination teams travelling by boat for hours to vaccinate a single child on a remote island.
“As a nurse, I had to contribute to prevent the spread of polio, a disease that we haven’t verified in the country for a long time,” said Tamara.
Two planned COVID-19 vaccination campaigns in 2022 failed to happen due to strikes by health workers, however plans were put in place during the year to hold the campaigns in 2023 to increase the coverage of fully vaccinated persons from the current 25 per cent of the entire population to 50 per cent, and for ‘single dose’ coverage to 38 per cent.

Malnutrition – a major public health challenge in Guinea-Bissau – is associated with high levels of maternal and child mortality. Wasting among children under the age of five is 5 per cent and 28 per cent of children of the same age group are stunted. These high levels of malnutrition are mainly due to limited knowledge of appropriate young child feeding practices, poor access to nutritious foods for young children; inadequate prevention and treatment of frequently occurring childhood illnesses, such as diarrhoea, pneumonia and malaria; and inadequate nutrition screening and care within communities and health-care facilities.
Guinea-Bissau has the highest HIV prevalence rate in West Africa – 3 per cent of people aged 15–49 years live with HIV – while the country’s antiretroviral therapy coverage is one of the lowest. Women are disproportionately affected.
Adolescent girls are particularly vulnerable, yet the coverage of antiretroviral treatment among pregnant women living with HIV decreased from 66 per cent in 2016 to 57 per cent in 2020.5
Key Results


Improving access to water, sanitation and hygiene

While open defecation prevalence decreased significantly from 36 per cent in 2000 to 10.3 per cent in 2020,1 disturbingly, access to safe water actually fell from 75 per cent in 2014 to 67 per cent in 2019.2 Currently, 55 per cent of water points and 82 per cent of household water sources are contaminated with faecal bacteria. Moreover, access to safe water could worsen in some areas due to climate change as rain patterns change, resulting in increased flooding, drought and salinization.
The most recent data (2019) showed nationally only 16 per cent of households have access to a place that has soap and water for handwashing.
Overall poor access to water, sanitation and hygiene (WASH) is a huge challenge leading to serious health conditions, such as cholera and diarrhoeal diseases. Diarrhoeal diseases remain the second leading cause of morbidity and mortality among children under the age of 5 in the country. Moreover, evidence has shown that poor WASH can hamper children’s recovery from malnutrition as a result of environmental enteropathy3 (UNICEF, World Health Organization, 2015). This can be especially serious for young children and can result in physical and cognitive stunting or death. Unsafe drinking water is also particularly serious for people living with HIV due to the increased risk of opportunistic infections.4
In addition, poor access to WASH is highly associated with malaria, polio and some of the World Health Organization’s neglected tropical diseases (NTDs) such as the guinea worm, schistosomiasis (bilharzia), soil-transmitted helminths (roundworm, whipworm and hookworm) and trachoma (a parasite that can cause blindness). These NTDs have a debilitating impact on children and their families and can harm a child’s physical and mental development.

